| Issue |
Radioprotection
Volume 53, Number 4, October-December 2018
|
|
|---|---|---|
| Page(s) | 287 - 291 | |
| DOI | https://doi.org/10.1051/radiopro/2018036 | |
| Published online | 16 November 2018 | |
Article
Comparative organ dose levels for dentomaxillofacial examinations performed with computed tomography, cone beam CT and panoramic radiographs
1
Institute of radiation physics, Lausanne University Hospital,
1 rue du Grand Pré,
1007
Lausanne, Switzerland
2
Department of Radiology, University Hospital of Geneva,
4 rue Gabrielle-Perret-Gentil,
1205
Geneva, Switzerland
3
Department of radiology, University of Otago,
Christchurch, New Zealand
* Corresponding author: This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
4
July
2018
Accepted:
29
October
2018
Abstract
The purpose of this study was to evaluate the radiation dose delivered to radiosensitive organs (thyroid, parotid glands and eye lens) during dentomaxillofacial imaging with multislice computed tomography (CT), cone beam CT (CBCT) and panoramic radiographs (orthopantomography, OPT). The dose was estimated individually for each modality and each clinical protocol by measuring the absorbed dose at the surface of a head phantom with thermoluminescence dosimeters. The measured radiation dose was between 0.01–1.22 mGy for the thyroid gland (systematically outside the primary beam), 1.34–29.11 mGy for the parotid glands (systematically exposed to the primary beam) and 0.02–26.22 mGy for the eye lens (in the primary beam depending on imaging protocol). For all organs, CT was found to be the most irradiating modality followed by CBCT and OPT. However, CBCT with a “limited dental” protocol and OPT deliver similar doses to the parotid glands.
Key words: dentomaxillofacial imaging / cone beam computed tomography / radiation dosimetry / orthopantomography / multislice computed tomography / organ absorbed doses
© EDP Sciences 2018
1 Introduction
Dentomaxillofacial examinations using X-rays have an important role in treatment planning, monitoring disease progression and assessing treatment efficacy. Performing dentomaxillofacial radiologic examinations results in irradiation of the thyroid gland, parotid gland and eye lens due to direct exposure to the X-ray beam or due to scatter irradiation. A large number of treated patients are children and young adults. Since only no exposure to X-rays can be considered free of risk, in particular for children (Pierce and Preston, 2000; Brenner, 2002), health professionals have the responsibility to ensure that the diagnostic value is maximized and the radiation doses are kept as low as reasonably achievable (European Commission, 2012).
Exposure of radiosensitive organs is influenced by the radiological modality used and the specific protocol applied. As a consequence, the choice of the modality is a very important issue. Panoramic radiography (orthopantomography, OPT) has been long considered as the examination method of choice for a variety of dental and maxillofacial applications. Compared with intraoral radiographs, OPT offers rapid overview of the dental arches, as well as detailed depiction of critical anatomical structures. However, this two-dimensional projection gives no information on bone thickness and provides less detailed information than bite-wing or intraoral radiographs (Muhammed and Manson-Hing, 1982). In addition, due to improper patient positioning and suboptimal image quality, OPTs can lead to diagnostic errors in a significant number of cases (Granlund et al., 2012). When risks of misdiagnosis and therapeutic uncertainties are present, three-dimensional information is required. Computed tomography (CT) allows extremely rapid data acquisition with excellent image resolution of the facial bones, skull base and dental structures. CT is used for the planning of interventions in the maxillofacial field, to anticipate surgical difficulties and to adapt the therapeutic strategy. However, despite recent technical advances, CT acquisitions have been traditionally associated with a relatively high radiation burden in comparison to cone beam CT (CBCT). Due to its low cost and easy accessibility, CBCT is currently performed for a variety of maxillofacial and dental applications, such as pre-operative implant planning, pre-operative imaging of impacted teeth, cysts and cyst-like lesions, and assessment of endodontic pathology (Guerrero et al., 2006; De Vos et al., 2009). The recent review and meta-analysis on CBCT by Ludlow et al. (2015) presents dose evaluation of dental imaging CBCT units (Ludlow et al., 2015). Although several publications have compared the radiation exposure of CT, CBCT and OPT, these articles have mainly focused on the total radiation exposure or have often compared radiation exposure based on protocols covering different anatomical areas.
The aim of the current study was to evaluate the radiation exposure of specific organs at risk applying similar volume coverage with CT, CBCT and OPT. Indeed, only organ or tissue radiation absorbed dose should be used for assessing the potential detriment for a patient. Effective dose has been first introduced by the ICRP to set limits for radiation protection and not to estimate future patient cancer risk from specific sources of radiation exposure (Fisher and Fahey, 2017). However, it could be used for comparing typical doses from different modalities, but this goes beyond the scope of the study.
2 Materials and methods
In this study, we compared three imaging systems in terms of organ dose levels for dentomaxillofacial examinations: a 64 multi-slice CT scanner (SIEMENS Somatom Definition Flash, Siemens, Erlangen, Germany), a CBCT (NewTom VGi, Quantitative Radiology, Verona, Italy) and an OPT (PlanMeca Promax S3, Planmeca, Helsinki, Finland). All systems had imaging protocols specifically developed for dentomaxillofacial examinations in clinical routine, providing the necessary image quality for diagnostic purposes and covering the same imaging volumes. Therefore, image quality was not specifically assessed during this study.
The dose at the entrance of three different radiosensitive organs (thyroid gland, parotid glands and eye lens) was evaluated. For this purpose, thermoluminescent dosimeters (TLDs) were taped on the surface of a phantom consisting of an adult skull embedded in transparent resin attached to a torso phantom of plastic containing all bone structures. In total 6 positions were considered, two for each organ (left and right). We are aware that the dose evaluated at the organ surface is a conservative approach and leads to slight overestimation of the exact dose value (ICRU, 2005) which depends on the beam quality. The chosen approach is, however, appropriate for the comparison between the different imaging modalities and protocols.
TLD-100 were used (LinatF, from Harshaw-Poland) to measure the absorbed dose. They were calibrated in an outside facility according to the accredited procedure. The energy correction factor of 0.77 was applied for measurements performed using CT and CBCT and of 0.70 for OPT, respectively.
The clinical protocols evaluated in the current study are routinely used in dentomaxillofacial imaging in our institution and provide adequate and similar image quality for the purpose of the respective clinical question. Protocol parameters are described in Table 1. Two CT protocols were available: a protocol referenced as “facial bones” covering the entire facial skeleton and with a large field of view (FOV), and a protocol referenced as “dental” covering only a small volume for limited dental assessment. Regarding CBCT, we use two dedicated protocols in clinical routine: a large FOV protocol registered under the name of “full” (Bornstein et al., 2014), and a medium size FOV protocol called “zoom” (Bornstein et al., 2014). A single protocol exists and was used for OPT (Tab. 1). The irradiation fields have been indicated for each modality and protocol on the phantom skull used for the measurements in Figure 1.
In order to reduce the uncertainty regarding the measured dose, repeat acquisitions were performed with the same set of TLDs for each modality and for each protocol. In total, 3 acquisitions were obtained for each CT protocol, 5 for each CBCT protocol and 10 for OPT. The measured values were subsequently normalized to be representative of the doses delivered for one single examination. The measurement error was evaluated to 10% (k = 2) for all modalities. Regarding OPT examinations, further measurements were performed over the period of this study in order to evaluate the homogeneity of the dose distribution. For those measurements, a raw of 5 TLDs spaced 2 cm was placed at each parotid gland.
Clinical protocol parameters used in routine imaging for each of the three modalities.
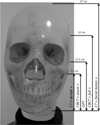 |
Fig. 1 Irradiation fields indicated for each modality and protocol on the phantom skull used for the measurements. |
3 Results
The absorbed dose at each radiosensitive organ considered in this study measured on the phantom’s surface is shown in Figure 2. Values are given for a single examination and for each modality and protocol. Because of the phantom used, the obtained values are representative for an adult.
For all organs and modalities, a left (L)/right (R) symmetry was noted. In all cases, the observed deviations were comparable with the error associated to the measurements performed with TLDs (estimated at 10%, not including errors due to slight differences in positioning).
The thyroid was the only organ systematically placed outside the primary beam. Its dose varied depending on the modality and protocol used. The largest dose values for this organ were obtained with CT, independently of the protocol chosen, with a maximum value = 1.22 mGy. The lowest value was obtained with OPT (0.01 mGy). The thyroid gland was clearly the least exposed organ among all studied organs.
The parotid gland was the only organ systematically located inside the primary radiation beam. Its exposure depended, as for the other organs, on the modality and the protocol used. The highest dose was measured at CT (highest value = 29.11 mGy) obtained for the protocol “facial bones”. For CBCT, parotid gland exposure was lower than with CT but it also strongly depended on the protocol used. The protocol “zoom” delivered the lowest dose (mean value = 1.44 mGy), which was equal to the mean dose received by this organ during OPT. The values for the parotid glands with OPT were the mean values of 5 TLDs at each parotid position. Indeed, for the OPT, the dose distribution around the parotids was found very inhomogeneous, with doses up to 45 times higher among two TLDs placed 2 cm apart as seen in Figure 3. For the OPT, the dose-width product (DWP) was evaluated by dividing the DAP value delivered by the equipment, by the slit length at the detector (Doyle et al., 2006).
The eye lens was in the primary beam for the CT protocol “facial bones” and for the CBCT protocol “full”. In these two cases, the doses were, as expected, higher than the ones observed for the other two protocols and for OPT. The highest dose was seen with CT (mean value = 25.46 mGy). When the lens was in the scattered beam, the trend was similar (higher dose with CT in comparison to CBCT and OPT, Fig. 2). OPT delivered the lowest dose to the eye lens (mean value = 0.02 mGy). This also demonstrates the importance of choosing the correct FOV for dose optimization (Pauwels et al., 2012).
In order to better compare radiation doses, the dose ratio was computed for the three organs at risk, for the different modalities and for the different protocols (Tab. 2).
 |
Fig. 2 Entrance dose at each radiosensitive organ for a single examination and for each modality and protocol. |
 |
Fig. 3 Entrance dose at the left parotid (TLDs 1 to 5) and at the right parotid (TLDs 6 to 10) for an OPT acquisition. |
Dose ratio for all three organs and for the different modalities. The values correspond to the mean values among the left/right organs and have been rounded to an integer.
4 Discussion
The absorbed doses measured at the phantom surface at the thyroid level were considerably lower than doses obtained for the other organs. For all modalities and protocols evaluated in this study, the thyroid was systematically outside the field of imaging and consequently was the only organ exposed to scattered radiation. However, the highest dose to the thyroid was measured for the “facial bones” protocol with CT. This can be explained by the proximity of the thyroid to the imaging area and hence, its proximity to the primary beam. In addition, the large beam of the CBCT compared to the slit beam of the OPT might be part of the explanation. For CT, measured doses were 6 to 10 times higher than for CBCT, and the lowest doses received by this organ were seen with OPT. The values we obtained for the thyroid, when irradiated with the CBCT protocol “full” are comparable to those reported by Al Najjar et al. (2013).
The parotid glands were the only organs systematically located in the primary beam area. For CT, the doses were 6 to 20 times higher than with all other modalities for the "facial bones" protocol and 9 times higher for the “dental” protocol. Our findings are in accordance to the findings reported by Suomalainen et al. (2009). The dose ratios CT/CBCT obtained in the current study varied between 6 and 9 and are again comparable to those reported by Suomalainen et al. (2009). We observed that the dose to the parotid glands was strongly influenced by the chosen protocol. The impact of a specific protocol on the parotid gland dose was also observed for CBCT, where the absorbed dose levels were 3 times higher for the “full” protocol than for the “zoom” protocol, the latter being similar to doses delivered by the mean values obtained with the OPT. However, as already mentioned, we observed that the OPT system tends to have strong dose inhomogeneity at the parotid level. The DWP value indicated by the equipment of 80 mGy.mm is compatible with the 76 mGy.mm reference value given by Williams and Montgomery (2000) and by Manousaridis et al. (2015). The reason for this inhomogeneity is the elliptical OPT trajectory, implying a higher intensity at the level of the temporomandibular joint. If instead of considering the mean dose among the 5 TLD placed at the parotid level, the highest dose value is considered for comparison between the two modalities, the level of parotid exposure obtained with OPT is comparable with the most irradiating CBCT protocol (protocol “full”). To the author’s knowledge this specificity of the OPT has never been mentioned before.
Regarding the eye lens, this organ is located outside of the examination area for OPT, for the CT protocol “dental” and for the CBCT protocol “zoom”. For this case where the eye lens is in the scattered field, the OPT delivers the lowest dose, CBCT follows with 13 times higher dose and the highest dose (approximate 12 times higher than CBCT) is obtained for CT. For the CBCT protocol “full” and for the CT protocol “facial bones", the eye lens is located in the field of examination and the radiation doses are ranging from 5.03 mGy to 26.22 mGy for each modality respectively. In this case, the dose of CT is only 5 times higher with respect to the dose delivered by CBCT. The values we obtained with CBCT are comparable with the range of dose values (0.03–16.7 mGy) reported by Pauwels (2015). In the case of a pediatric patient, the eye lens would potentially be in the primary beam for all modalities and protocols.
5 Conclusion
Due to its position systematically outside de primary beam, the thyroid is the least exposed organ for all modalities and protocols. In the contrary, the parotid is the organ systematically exposed for all modalities and protocols. Its dose depends on the modality and protocol chosen. The highest radiation exposure corresponds to CT examinations followed by CBCT with the protocol “full”. OPT together with the CBCT protocol “zoom” deliver the lowest dose values. For the eye lens, when the eye lens is located outside the primary beam the most irradiating modality is CT, followed by CBCT and OPT. When the organ is placed inside the primary beam, the same trend is observed excluding OPT since for this modality the eye lens is systematically outside the primary beam.
Acknowledgements
We would like to thank Cesare Zingariello and François Riondel for their help during the measurements, without them this work would not have been possible. Special thanks to Juha Koivisto for providing the explanation regarding radiation inhomogeneity observed for the OPT modality.
References
- Al Najjar A, Colosi D, Dauer LT, Prins R, Patchell G, Branets I, Goren AD, Faber RD. 2013. Comparison of adult and child radiation equivalent doses from 2 dental cone-beam computed tomography units. Am. J. Orthod. Dentofac. Orthop. 143(6): 784–792. [CrossRef] [Google Scholar]
- Bornstein MM, Scarfe WC, Vaughn VM, Jacobs R. 2014. Cone beam computed tomography in implant dentistry: a systematic review focusing on guidelines, indications, and radiation dose risks. Int. J. Oral Maxillofac. Implants. 29(Suppl): 55–77. [CrossRef] [PubMed] [Google Scholar]
- Brenner DJ. 2002. Estimating cancer risks from pediatric CT: going from the qualitative to the quantitative. Pediatr. Radiol. 32: 228–233. [CrossRef] [PubMed] [Google Scholar]
- De Vos W, Casselman J, Swennen GR. 2009. Cone-beam computerized tomography (CBCT) imaging of the oral and maxillofacial region: a systematic review of the literature. Int. J. Oral Maxillofac. Surg. 38(6): 609–625. [Google Scholar]
- Doyle P, Martin CJ, Robertson J. 2006. Techniques for measurement of dose width product in panoramic dental radiography. Br. J. Radiol. 79: 142–147. [CrossRef] [PubMed] [Google Scholar]
- European Commission. 2012. Radiation Protection no172, Cone beam CT for dental and maxillofacial radiology (Evidence-based guidelines). ISSN 1681–6803. [Google Scholar]
- Fisher DR, Fahey FH. 2017. Appropriate use of effective dose in radiation protection and risk assessment. Health Phys. 113(2): 102–109. [CrossRef] [PubMed] [Google Scholar]
- Granlund CM, Lith A, Molander B, Gröndahl K, Hansen K, Ekestubbe A. 2012. Frequency of errors and pathology in panoramic images of young orthodontic patients. Eur. J. Orthod. 34(4): 452–457. [CrossRef] [PubMed] [Google Scholar]
- Guerrero ME, Jacobs R, Loubele M, Schutyser F, Suetens P, van Steenberghe D. 2006. State-of-the-art on cone beam CT imaging for preoperative planning of implant placement. Clin. Oral Invest. 10: 1–7. [CrossRef] [PubMed] [Google Scholar]
- ICRU. 2005. Patient dosimetry for X-rays used in medical imaging (Report 74). J. ICRU 5(2): iv–vi. [Google Scholar]
- Ludlow JB, Timothy R, Walker C, Hunter R, Benavides E, Samuelson DB, Scheske MJ. 2015. Effective dose of dental CBCT – a meta analysis of published data and additional data for nine CBCT units. Dentomaxillofac. Radiol. 44: 20140197. [CrossRef] [PubMed] [Google Scholar]
- Manousaridis G, Koukorava C, Hourdakis CJ, Kamenopoulou V, Yakoumakis E, Tsiklakis K. 2015. Establishment of diagnostic reference levees for dental panoramic radiography in Greece. Radiat. Prot. Dosim. 165(1–4): pp. 111–114. [CrossRef] [Google Scholar]
- Muhammed AH, Manson-Hing LR. 1982. A comparison of panoramic and intraoral radiographic surveys in evaluating a dental clinic population. Oral Surg. Oral Med. Oral Pathol. 54(1): 108–117. [CrossRef] [PubMed] [Google Scholar]
- Pauwels R. 2015. Cone beam CT for dental and maxillofacial imaging: dose matters. Radiat. Prot. Dosim. 165(1–4): 156–161. [CrossRef] [Google Scholar]
- Pauwels R, Theodorakou C, Walker A, Bosmans H, Jacobs R, Horner K, Bogaerts R, The SEDENTEXCT Project Consortium. 2012. Dose distribution for dental cone beam CT and its implication for defining a dose index. Dentomaxillofac. Radiol. 41: 583–593. [Google Scholar]
- Pierce DA, Preston DL. 2000. Radiation-related cancer risks at low doses among atomic bomb survivors. Radiat. Res. 154: 178–186. [CrossRef] [PubMed] [Google Scholar]
- Suomalainen A, Kiljunen T, Käser Y, Peltola J, Kortesniemi M. 2009. Dosimetry and image quality of four dental cone beam computed tomography scanners compared with multislice computed tomography scanners. Dentomaxillofac. Radiol. 38: 367–378. [CrossRef] [PubMed] [Google Scholar]
- Williams JR, Montgomery A. 2000. Measurement of dose in panoramic dental radiology. Br. J. Radiol. 73: 1002–1006. [CrossRef] [PubMed] [Google Scholar]
Cite this article as: Sans Merce M, Damet J, Becker M. 2018. Comparative organ dose levels for dentomaxillofacial examinations performed with computed tomography, cone beam CT and panoramic radiographs. Radioprotection 53(4): 287–291
All Tables
Clinical protocol parameters used in routine imaging for each of the three modalities.
Dose ratio for all three organs and for the different modalities. The values correspond to the mean values among the left/right organs and have been rounded to an integer.
All Figures
 |
Fig. 1 Irradiation fields indicated for each modality and protocol on the phantom skull used for the measurements. |
| In the text | |
 |
Fig. 2 Entrance dose at each radiosensitive organ for a single examination and for each modality and protocol. |
| In the text | |
 |
Fig. 3 Entrance dose at the left parotid (TLDs 1 to 5) and at the right parotid (TLDs 6 to 10) for an OPT acquisition. |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.




